Time is brain: What to know about stroke
(BPT) - For every minute a stroke goes untreated, an estimated 1.9 million brain cells diei- damage that can quickly become permanent and lead to long-term disability or death. It's why medical experts repeat the phrase "time is brain." When a stroke strikes, every second carries life-altering consequences.
According to the Centers for Disease Control and Prevention, strokes are common and can be devastating for patients and their families. In the United States, a stroke occurs every 40 seconds,ii and someone dies from one about every three minutes.iii Each year, more than 795,000 Americans have a stroke, making it a leading cause of serious long-term disability.iv In fact, more than half of survivors aged 65 and older have ongoing difficulty with movement afterward. Beyond the personal toll, strokes cost the U.S. nearly $56.2 billion in healthcare expenses and lost productivity from 2019 to 2020.v
Common risk factors for stroke include high blood pressure, diabetes, smoking and obesity - many of which are manageable with lifestyle changes and medical care. Even though risk goes up with age, more younger adults are being affected as these issues become more widespread.vi
Recognizing stroke symptoms: Think B.E. F.A.S.T.
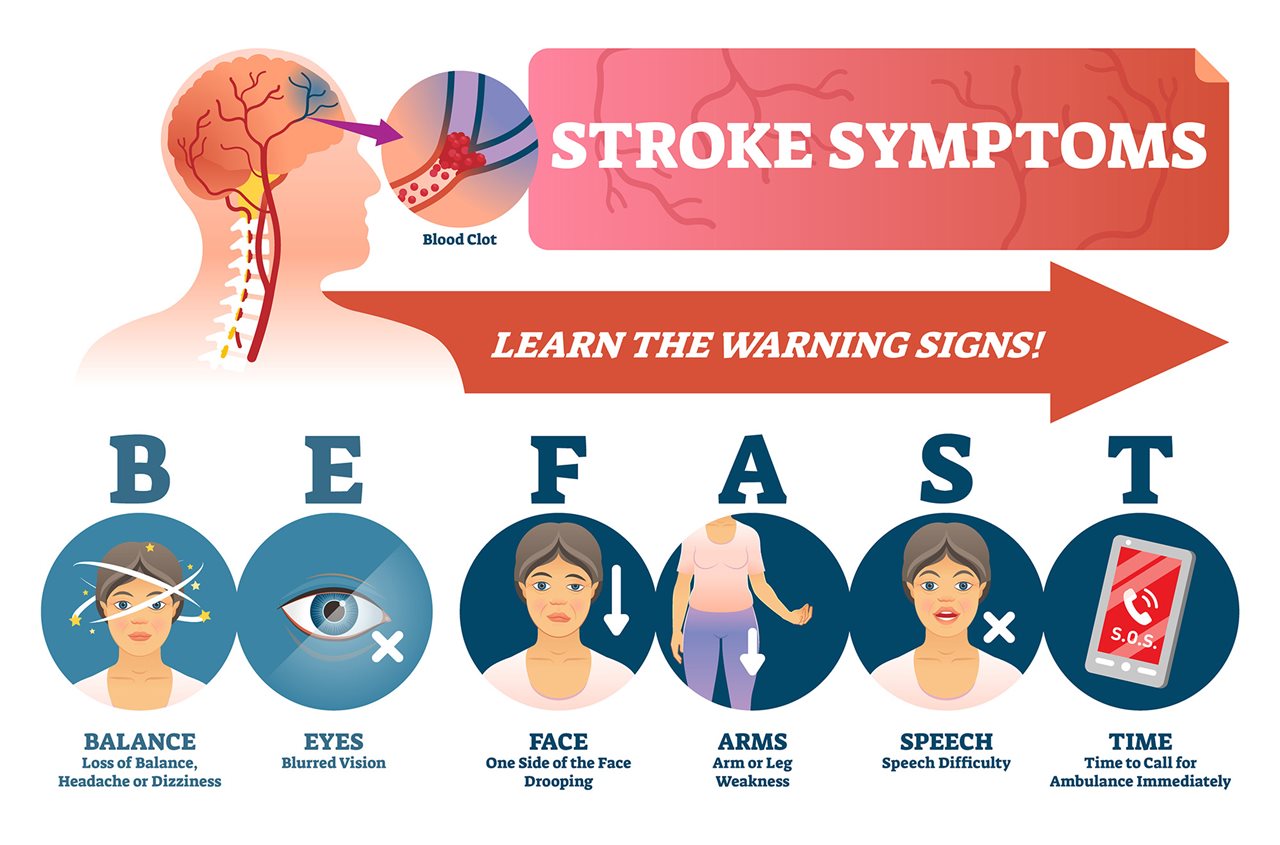
For all of these reasons, early recognition of a stroke is critical. The sooner treatment begins, the greater the chances of survival and meaningful recovery. Health experts recommend the B.E. F.A.S.T. acronym as a simple, effective tool for identifying the most common warning signs:
- Bfor Balance Loss: Sudden dizziness, loss of coordination, or trouble walking.
- Efor Eye (Vision) Changes: Sudden blurred, double or lost vision in one or both eyes.
- Ffor Face Drooping: One side of the face droops or feels numb - ask the person to smile and look for unevenness.
- Afor Arm Weakness: One arm feels weak or numb - ask the person to raise both arms and watch for one drifting downward.
- Sfor Speech Difficulty: Slurred or confused speech - ask the person to repeat a simple sentence.
- T for Time to Call 911: Call emergency services immediately. When in doubt, act - the cost of waiting is far greater than the cost of a false alarm.
Additional warning signs include sudden confusion, a severe headache with no known cause, and numbness or weakness on one side of the body.
Finding a stroke center before an emergency

Beyond recognizing symptoms, one of the most valuable steps individuals and families can take is identifying the nearest certified stroke center before an emergency occurs as it could save critical minutes when a stroke happens.
Comprehensive Stroke Centers are hospitals specially equipped to provide the highest level of stroke care. Certified by organizations like The Joint Commission, they offer 24/7 care and are equipped with the tools needed to diagnose and treat strokes quickly. Many regions also have Primary Stroke Centers or Thrombectomy-Capable Stroke Centers that provide specialized, timely treatment.
To find a nearby stroke-ready hospital:
- Use hospital locator tools provided by the The Joint Commission (www.jointcommission.org) or the American Stroke Association (www.stroke.org)
- Check with your local health department or major hospital systems
- Ask your primary care provider about the closest certified facility
While emergency medical services will typically transport patients to the nearest appropriate hospital, knowing the closest certified stroke center in advance empowers families to advocate quickly when every second matters.
Latest advancements offer new hope

While prevention and rapid response are critical, advances in treatment are improving survival and recovery rates - particularly for acute ischemic stroke, the most common type of stroke.
One of the latest advancements is mechanical thrombectomy, which is a minimally invasive procedure that removes blood clots from the brain to restore circulation. A type of mechanical thrombectomy is aspiration thrombectomy, done with products such as Penumbra's RED Reperfusion Catheters, which uses a vacuum to remove clots from blocked blood vessels and restores blood flow quickly.
Clinical studies show mechanical thrombectomy works faster and is more likely to restore blood flow compared to other treatments such as thrombolysis - a procedure that uses clot-busting medication (such as tPA) to dissolve dangerous blood clots in arteries or veins and restore blood flow.vii
With a stroke occurring somewhere in the United States every 40 seconds, the message is clear: Recognizing the symptoms, calling 911 and knowing where to go as well as your treatment options aren't just good practices - they're lifesaving ones.
ii Tsao CW, Aday AW, Almarzooq ZI, et al. Heart disease and stroke statistics-2023 update: a report from the American Heart Association. Circulation. 2023;147:e93-e621.
iii National Center for Health Statistics. Multiple Cause of Death 2018-2023 on CDC WONDER Database. Accessed February 1, 2025. https://wonder.cdc.gov/mcd.html
iv Tsao CW, Aday AW, Almarzooq ZI, et al. Heart disease and stroke statistics-2023 update: a report from the American Heart Association. Circulation. 2023;147:e93-e621.
v Martin SS, Aday AW, Almarzooq ZI, et al.; American Heart Association Council on Epidemiology and Prevention Statistics Committee; Stroke Statistics Subcommittee. 2024 heart disease and stroke statistics: a report of US and global data from the American Heart Association. Circulation 2024;149:e347-913.
vi Centers for Disease Control and Prevention. Prevalence of Stroke - Behavioral Risk Factor Surveillance System, United States, 2011-2022. MMWR Morb Mortal Wkly Rep. 2024;73(20). https://www.cdc.gov/mmwr/volumes/73/wr/mm7320a1.htm
vii Bekele BA, Uwishema O, Adam AH, Gashu AD, Kachouh C, Mshaymesh S, Wellington J. Comparative effectiveness of intra-arterial thrombolysis vs. mechanical thrombectomy: a literature review. Ann Med Surg (Lond). 2025 Apr 16;87(5):2749-2757. doi: 10.1097/MS9.0000000000003139. PMID: 40337416; PMCID: PMC12055068. https://pmc.ncbi.nlm.nih.gov/articles/PMC12055068/
Caution: Federal (USA) law restricts these devices to sale by or on the order of a physician. Prior to use, please refer to the Instructions for Use for complete product indications, contraindications, warnings, precautions, potential adverse events, and detailed instructions for use. For the complete Penumbra IFU Summary Statements, please visit www.peninc.info/risk. Please contact your local Penumbra representative for more information.
Source: BrandPoint